Why "Personal Belief" Vaccine Exemptions Place Many Vulnerable Americans at Risk
For good reason, childhood vaccination programs top the Center for Disease Control’s list of “Ten Great Public Health Achievements” of the 20th century. Early in the 20th century there were almost 50,000 smallpox cases reported each year with a 30 percent mortality rate, but the United States reported none by 1949. Polio was eradicated in the Western Hemisphere by 1991, preventing more than 2,000 U.S. polio-related deaths every year; and the infant Haemophilus influenza vaccine has reduced by more than 99 percent the former leading cause of post-natal mental retardation. Unfortunately, despite these huge gains, anti-vaccine rhetoric and pervasive false claims now threaten to erode public trust in the safety and effectiveness of vaccine programs.
Compounding the effect of this distrust, dozens of U.S. states have enacted laws to permit non-medical, or “personal belief” exemptions to childhood vaccinations. These laws, while seeking to protect individual liberties, open the door to concentrated, like-minded communities of unvaccinated or under-vaccinated individuals. In turn, these communities become increasingly susceptible to disease outbreaks, and undermine what is called “herd immunity”. The loss of herd immunity places the general population at risk, and is especially devastating for infants, the elderly, and those with compromised immune systems who cannot be effectively vaccinated.
How Herd Immunity Works
Vaccinations prime an individual’s immune system to recognize a specific infectious pathogen. If the vaccine is effective, the individual’s immune system will generate a robust anti-vaccine response that will protect him/her from infection with the ‘real’ disease. Most people in any given community can be protected this way, but not all. Because immune function varies highly between individuals, even a well-designed vaccine will fail to protect a number of healthy, middle-aged people. Moreover, infants with undeveloped immune systems and people with aging or compromised immune systems, such as cancer or AIDS patients, are unable to generate these robust responses and do not directly benefit from vaccination. Unfortunately, these same individuals are also the most vulnerable to disease, and are more likely to experience severe complications or even death if they become infected.
Fortunately, vaccination campaigns are designed to protect entire communities. For example, even though 12 percent of people do not acquire individual immunity against mumps from the measles, mumps and rubella vaccine, the campaign has achieved a 99.8 percent reduction in the number of mumps cases overall. Strong protection is accomplished through herd immunity – when, as illustrated below – almost everyone is vaccinated who safely can be. A ring of protection is built around vulnerable individuals who cannot be successfully individually vaccinated.
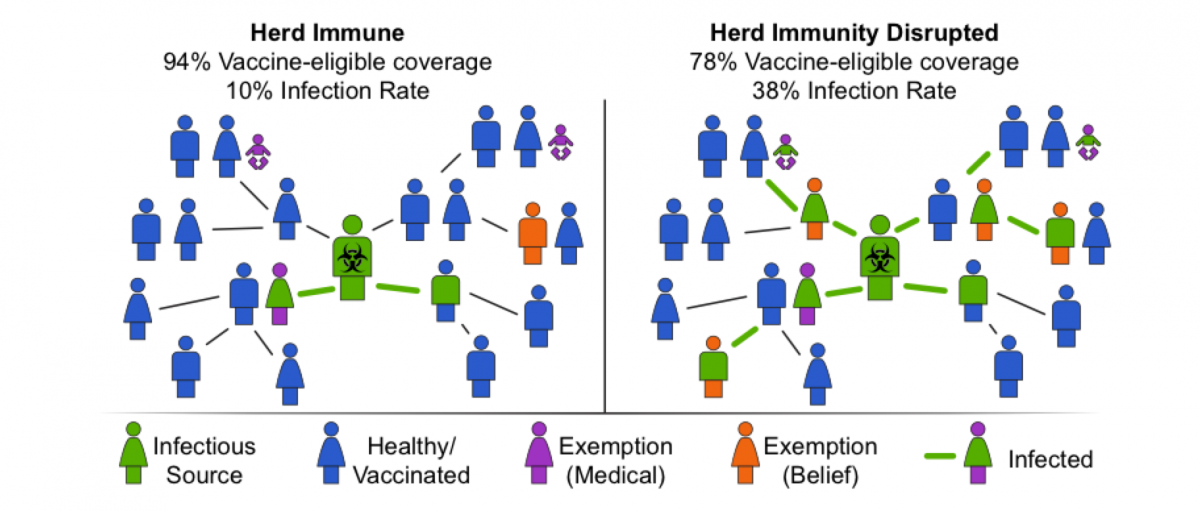
Loss of Herd Immunity Disproportionately Harms Vulnerable Populations
As of August, 2016, 47 states allowed some form of non-medical vaccination exemption for reasons ranging from religious beliefs to simple personal objections to vaccination. With misinformation about the safety of vaccines spreading, increasing numbers of parents exploit these exceptions to avoid vaccinating their children. More troubling, public health studies consistently show that parents that choose not to vaccinate tend to cluster within communities, creating unvaccinated islands that are conducive to infectious outbreak.
Analyses of new measles outbreaks occurring since January, 2000 have found that outbreaks often occur within under-vaccinated communities, where more than 70 percent of unvaccinated people cited personal belief as their reason for non-vaccination. But those who refused vaccinations are not the only ones affected – almost 60 percent of the resulting infections occurred in individuals that either were vaccinated, or could not be due to medical reasons. Stated another way, non-medical exemptions disproportionately affect individuals that either could not protect themselves through vaccination due to a medical condition, or were vaccinated but not effectively protected.
Vaccine Coverage Must be Strengthened
It is imperative that the United States take steps to continue vaccine coverage needed to protect those most vulnerable to infection. Non-medical, personal belief exemptions should be eliminated through state or federal legislation. By requiring vaccinations for all children prior to enrollment in public or private schools, gaps in coverage due to poor choices by like-minded parents can be eliminated and infectious disease protection can be extended to everyone, including the most vulnerable. The courts have long upheld this type of vaccination mandate, which has been highly effective in California, West Virginia, and Mississippi.
Beyond legislation, new public education efforts must counter false claims that vaccines are unsafe and explain why they are critical to public as well as personal health. By creating an environment where individuals understand their responsibilities to community health, America can protect the vulnerable and solidify the enormous health benefits we have achieved through vaccination.
